COVID-19 Associated Cutanous Small-Vessel Vasculitis
COVID-19 is caused by SARS-CoV-2 and is a public health emergency worldwide. Infection associated cutaneous manifestations are being increasingly reported and classified according to clinical findings in exanthematic or vasculitic process. We report the case of a 75-year-old female patient with hospital-acquired COVID19 infection, with mild form of disease. 18 days after beginning of symptoms the patient develops palpable purpura on both knees compatible with small-vessel cutaneous vasculitis, with full recovery. We emphasize the need for documentation of infection-associated vasculitic processes for better recognition on clinical practice.
Keywords:COVID-19; Purpura; Hypersensitivity Vasculitis
COVID-19 is caused by SARS-CoV-2 and is a public health emergency worldwide. Although its pathogenesis is not entirely understood, it has multisystemic involvement, mainly affecting the respiratory system, digestive tract and cranial nerves [1]. Lately, COVID-19 cutaneous manifestations are being increasingly reported, some in the form of vasculitis. Viral infection has been long known as a vasculitis cause. However, little is known about skin histopathological features or if SARS-CoV-2 is present on the lesions [2, 3]. The authors present a case of COVID-19 associated small vessel cutaneous vasculitis.
This was a comparative cross sectional study. The study was conducted at Department of Paediatric Neurology, Bangabandhu Sheikh Mujib Medical University, Dhaka from July 2017 to June 2018.Total 102 patients were selected consecutively following the inclusion and exclusion criteria. Evaluations of patients were based on history, physical examination and neurodevelopment assessment. For analysis of results patients were divided into two groups: case-68 and control-34.
75-year-old female patient with a history of chronic gastritis and heart failure with reduced left ventricular ejection fraction with a class IV of NYHA (New York Heart Association), of ischemic origin. The patient had a myocardial infarction complicated with left ventricle free wall rupture, and underwent cardiac left ventriculoplasty and mitral and tricuspid annuloplasty. 18 days after surgery she tested positive for SARS-CoV-2 (nasal swab RT-PCR) after high-risk contact – hospital-acquired infection. Progressed with a mild form of disease: slight worsening of dyspnea at rest and dry cough, with symptom onset at the time of diagnosis. (4) Analytical parameters showed a maximum of 103,5mg/L C-Reactive Protein (C-RP) at time of diagnosis, with decrease for 18 days and recrudescence to 36mg/L and normalization thereafter; maximum ferritin of 380,39 ng/mL, lactic dehydrogenase (LDH) of 263U/L and d-dimer of 3666ng/mL, at diagnosis. Chest CT scan, 6 days after diagnosis, revealed scarce peripheral and peribronchovascular ground glass opacities on the left lung and apical right lung compatible with viral pneumonia.
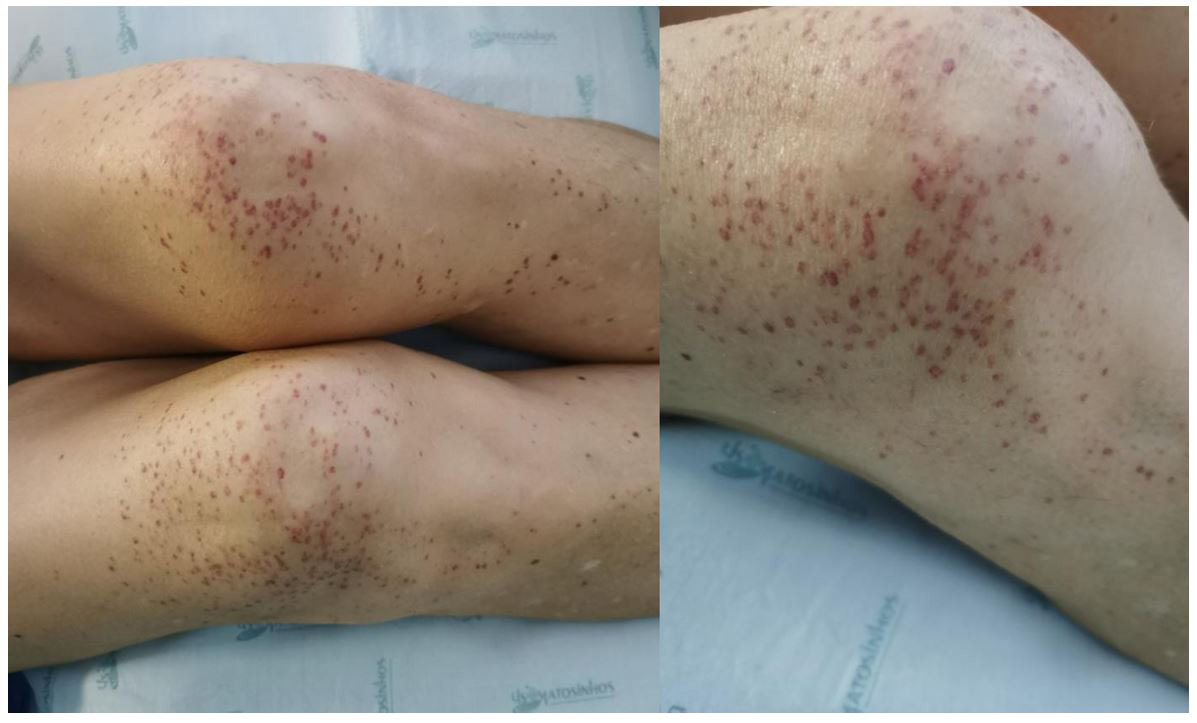
13 days after diagnosis the patient developed bilateral knee pruritic erythema, that in 5 days evolved to palpable purpura (Figure 1). No nodules, livedo reticular, ulcers, retiform purpura or necrosis were found. No visceral vasculitic involvement was evident and no arthralgias were present. Neurological, hepatic and renal function were unaltered. No new drugs were initiated in the 15 days prior to lesion development. She was medicated with warfarin, 100mg of acetylsalicylic acid, 5mg of diazepam, 80mg of oral furosemide, 20mg of pantoprazole and 10mg of rosuvastatin.
Etiological study showed an increased sedimentation rate of 105mm/1h, negative serology for syphilis, cytomegalovirus (CMV), Epstein-Barr virus (EBV), human immunodeficiency virus (HIV), hepatitis B and C (HBV vaccinated) and parvovirus B19. Anti-nuclear antibodies (ANA, anti-dsDNA, anti-ENA) and Anti- neutrophil cytoplasm antibodies (ANCA anti-PR3 e anti-MPO) search was negative. Rheumatoid factor dosing was <12,0 UI/mL and IgG was slightly increased with 1698mg/dL [552-1631 reference range] with normal IgA. Complement (C3 and C4) dosing was also normal.
Skin biopsies were performed 4 days after appearance of palpable purpura with the patient already on treatment. Histology showed unspecific slight perivascular lymphocytic inflammatory infiltrate on the dermis.
A diagnosis of SARS-CoV-2 infection associated small vessel cutaneous vasculitis was established. The patient didn´t do any COVID-19 specific treatment and had total symptom resolution. Purpuric lesions disappeared after 14 days. Betamethasone 0,1% cream was applied twice a day.
SARS-CoV-2 can affect any organ or system, and being a newly identified virus, several clinical manifestations are still being reported and studied [2]. Unfortunately, most retrospective studies on COVID-19 cutaneous manifestations lack histological analysis that allow to take conclusions on pathological features and pathognomonic findings 2]. To date, skin lesions have been classified according to clinical findings in exanthematic or associated with vasculitic process [5-7]. The second group includes: digital ischemia (more frequent in children and adolescents), bullae, gangrene, livedo reticular, chilblains and purpura [6, 7].
Castelnovo et al report a patient with critical form of disease, that develops palpable purpura affecting the legs, evolving to erythematous rash and resolution after a few days with topical corticosteroid [8].
Tahir, et al. describe a case with appearance of skin lesions 3 days prior to respiratory symptoms, in a mild form of disease. The lesions involved the legs, arms and thorax. Initially the lesions appeared as red to purple plaques evolving with necrotic center and areas of palpable purpura. Biopsy of one of the plaques revealed dermal perivascular infiltrate, endothelial cell swelling, neutrophilic infiltration of vessel wall, extravasated erythrocytes and microthrombi occluding the lumina of the smaller capillaries in the dermis [9].
Caputo et al published one of the first cases of histologically confirmed cutaneous small vessel vasculitis. The patient had a critical form do COVID-19 infection requiring mechanical ventilation support. On the 35th day of hospitalization he developed a diffuse purpuric rash with skin biopsy compatible with small vessel vasculitis. In this case there was a clinical suspicion of neurological involvement [10].
Dominguez-Santas et al present a case very similar to ours, with palpable purpura appearing on both legs. Onset was 7 days after respiratory symptoms. A skin biopsy confirmed small vessel vasculitis. Topical corticosteroid was applied and complete resolution was obtained after 3 weeks [3].
There is a tendency for skin lesions to appear after respiratory symptoms onset [7]. Disease severity does not seem to be related with cutaneous involvement, since they are reported in all clinical spectrum. Time to resolution of skin lesions is reported between hours to 3 weeks [6, 7, 8]. In most cases either topical corticosteroid was applied or no treatment [3, 8, 9].
We present a case of cutaneous small vessel vasculitis associated with SARS-CoV-2 infection, in a mild form of disease, with onset 18 days after respiratory symptoms, and resolution after 14 days. Although no pathognomonic histological features are described, this was the most likely clinical scenario given the exclusion of other etiologies such as virus, autoimmunity or drugs.
Cutaneous manifestations, particularly vasculitic processes, associated with COVID-19 are rarely reported and likely underdiagnosed. We emphasize the need for documentation for better recognition on clinical practice.