Delayed Pericardial Tamponade after Nail Gun Injury to the Right Ventricle
The use of nail guns has been expanded since 1950s, as it requires a minimum training. Nail guns can fire projectiles at a rapid speed for a distance up to 500 meters. Cardiac nail gun injuries are rare but life-threatening. Most of the cases presented within few minutes after injury and associated with hemodynamic compromise and some degree of pericardial tamponade. We describe a case of 19-years-old carpenter presented 15 hours after nail gun injury without hemohynamic compromise. Chest CT detected penetration of the nail tip in the pericardium with pericardial effusion. The hemodynamic status deteriorated during diagnostic workup. The bedside echocardiography revealed tamponading pericardial effusion. Through the left anterior thoracotomy, intrapericardial hematoma was removed, the nail was successfully extracted, and a laceration in the right ventricle was repaired. The postoperative course was uneventful. In conclusion, nail gun should be considered as one of the essential causes of penetrating cardiac injury. High index of suspicion and appropriate imaging studies result in successful management of hemodynamically stable patients. An aggressive approach without time consuming investigations is preferred for unstable patients after penetrating cardiac injury.
Keywords: Cardiac Injury; Nail Gun Injury; Penetrating Trauma; Pericardial Tamponade
Penetrating cardiac injury is an emergent condition which has a high rate of mortality. Alive patients have a variable clinical presentation at the emergency department with a pericardial tamponade in 70% of survivors and 20% of non-survivors [1]. Firearm and stab wounds are the most common causes of penetrating cardiac injury [2].
Nail guns have been used since 1950s to fire nails into woods, concrete and metal surfaces, with the ability to fire projectiles at a speed of 100-150 meters/second and distances of up to 500 meters [3]. Increasing the use of nail guns, as it requires a minimum training, has been reported to increase the rate of nail gun injuries [4]. Extremities are the most common site susceptible to accidental trauma, while penetrating cardiac injury is much less common injury secondary to discharge of pneumatic nail gun [5].
Nail gun cardiac injuries are fairly rare entity, mostly reported in adult males, due to working related infliction with a nail with a death risk of 25% [6]. Searching Medline on July 2018 determined only 25 published case reports of nail gun cardiac injuries. In most of the reported cases, patients survive as the nail wedges in the soft tissue even when there is a chamber injury. Eleven case reports, described 13 patients presented with stable hemodynamic status or had delayed presentation after cardiac nail gun injuries (Table 1).
We reported a rare case with delayed presentation of pericardial tamponade after cardiac nail gun injury. We described clinical features, results of imaging studies, surgical procedure and postoperative outcome. Also, we review the literature by searching MEDLINE for similar cases of cardiac nail gun injuries using keywords of (cardiac injury) and (nail gun).
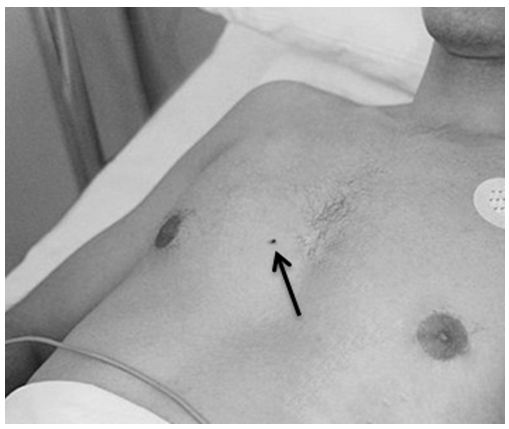
A 19-years-old male presented at the emergency department 15 hours after nail gun injury during his work as a carpenter. The patient did not notice the entrance of the nail and he thought it hit him and came on the ground. He asked for medical advice at a primary care center after development of severe chest pain, where he was referred to our university hospital. The physical examination revealed pinpoint skin wound at the right side of the sternum along the intermammary line (Figure 1). The patient was fully conscious and his vital signs were: blood pressure 90/60 mm Hg, heart rate 100 beats/min, and respiratory rate 18 breaths/min. Peripheral venous and arterial lines and urinary catheter were inserted.
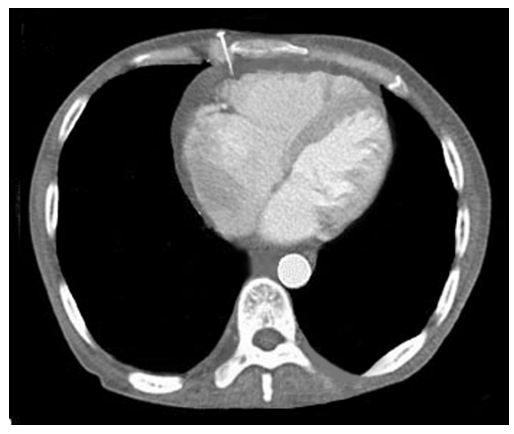
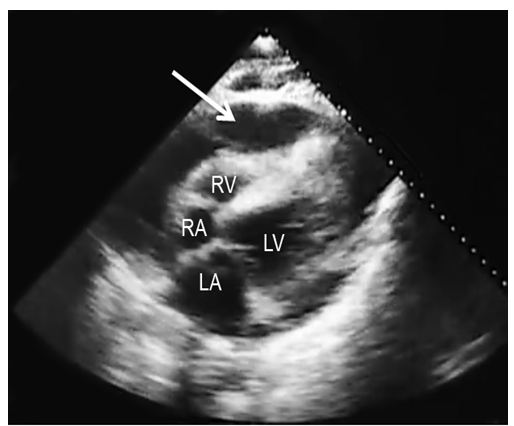
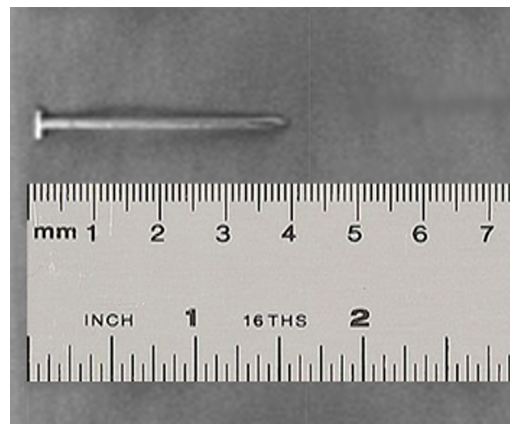
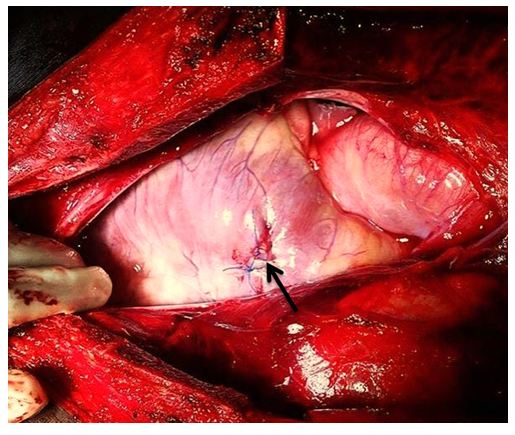
Computed tomography (CT) scan was performed and revealed right parasternal nail penetrating through the soft tissue, costal cartilage and pericardium associated with pericardial effusion (Figure 2). After CT scanning, the patient became drowsy with deterioration of vital signs: blood pressure 85/50 mm Hg, heart rate 110 beats/min, and respiratory rate 20 breaths/min. Bedside echocardiography revealed tamponading pericardial effusion with collapse of the right ventricle during diastole (Figure 3). Thereafter, the patient was transferred immediately to the operating room. Left anterior thoracotomy revealed penetration of the nail tip into pericardium through a small hole, with hemopericardium and large hematoma over the right side of the heart. After evacuation of the hematoma, a small puncture at the anterior surface of right ventricle was observed and started to re-bleed after removal of the hematoma. The bleeding from the puncture was initially controlled by digital pressure. A 4-cm nail (Figure 4) was removed outward through its track from the pericardium, costal cartilage and soft tissue. The direct repair of the right ventricular injury was performed with two 3/0 Prolene sutures (Figure 5). The patient developed no post-operative complications and he was discharged home at the 5th day after surgery.
Cardiac nail gun injury is a rare work-related hazard associated with 25% risk of mortality in male adults [6]. Most of these injuries are a result of accidental discharge of nail gun, commonly involve the right ventricle due to its anterior location, and associated with variable degrees of pericardial tamponade [7].
The clinical presentation of survivors varies in regard to their hemodynamic stability [8]. Most of the reported cases presented few minutes after trauma. Rare cases of delayed presentation or stable hemodynamic status at admission after cardiac nail gun injury were previously reported (Table 1) [5, 8,17]. There is no standard reason for delayed presentation, but it could be related to stable hemodyamic status and invisible non-bleeding pinpoint skin wound [8,13]. In our case, the delayed presentation of pericardial tamponade after accidental nail gun injury is related to absence of annoying symptoms after trauma. The nail wedged in the soft tissue, costal cartilage and pericardium without a complete penetration through the cardiac chambers. The tip of the nail hit the right ventricle during cardiac movement causing a small puncture followed by gradual bleeding and formation of intra-pericardial hematoma.
Delayed pericardial tamponade after penetrating cardiac injury is a challenging diagnostic and therapeutic entity, with several proposed mechanisms including clot sealing a partial tear associated with slow leak into pericardium or sudden dislodgment followed by rapid accumulation of blood [18]. In stable patients and in those with unclear presentation, imaging modalities particularly echocardiography have a vital role to confirm the presence of pericardial tamponade [13]. Chest computed tomography (CT) scans can be used to confirm the intra-thoracic position of the nail, and to detect pericardial effusion [8]. The stable status of our case at admission gave us the chance to perform preoperative CT and bedside echocardiography [14-17].
A controversy remains regarding the conservative management and pericardiocentesis in patients with no tamponade and stable hemodynamic status. Percardiocentesis can serve as a temporary life-saving measure, particularly as a bridge to definitive therapy [18,19]. The presence of pericardial tamponade indicates an emergent surgical intervention via median sternotomy or thoracotomy according to the location of cardiac injury [20]. Emergency department thoracotomy is favored for the hemodynamically unstable or pulseless patient [19]. In our case with unusual presentation, we preferred anterior thoracotomy in the operating room as the hemodynamic status was query stable and the imaging studies excluded penetration of the nail into cardiac chambers or major blood vessels.
Adequate training and applying of the security systems are essential to prevent accidental nail gun injuries. In addition to firearm and stab wounds, nail gun is an essential cause of penetrating cardiac injury. Cardiac nail gun injury is a rare emergency condition requires early diagnosis and immediate intervention to reduce the rate of mortality. High index of clinical suspicion and use of the best and fastest imaging modalities are useful for successful management of stable patients. Unstable hemodynamic status after penetrating trauma to the cardiac box raises the alert for pericardial tamponade. Aggressive approach with proper resuscitation and avoid of time consuming investigations are crucial for unstable patients with penetrating cardiac injury.